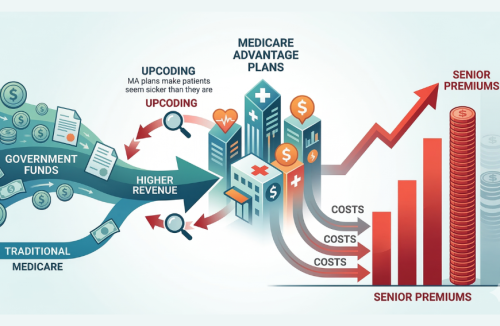
Medicare premiums are projected to rise sharply over the next decade, threatening to erode the retirement income of millions of American seniors. Much of the discussion about these increases focuses on the rising cost of healthcare itself. But an important and largely overlooked driver of higher premiums lies in how Medicare Advantage plans are paid.
According to projections from the Medicare Trustees, per-person spending in Medicare Part B — which covers physician services, outpatient care and many medications — is expected to nearly double over the next decade, rising from roughly $9,100 per beneficiary in 2025 to more than $18,000 by 2035. Because federal law requires Medicare premiums to cover approximately 25 percent of Part B costs, the average annual premium could rise from about $2,400 today to roughly $5,000 within ten years.
However, healthcare inflation alone does not explain why seniors are paying more. A growing share of these higher costs is tied to the way Medicare Advantage (MA) plans are reimbursed.
Medicare Advantage was originally designed to save money. When Congress expanded the program, the expectation was that private insurers could deliver care more efficiently than traditional fee-for-service Medicare. Policymakers initially envisioned paying private plans about 95 percent of the cost of Traditional Medicare, allowing taxpayers and beneficiaries to share in the savings. Instead, the opposite has occurred.
The independent Medicare Payment Advisory Commission now estimates that Medicare Advantage plans are being paid about 120 percent of what it would cost to cover the same beneficiaries under Traditional Medicare. In 2025 alone, those additional payments are projected to total roughly $84 billion.
READ: Sreedhar Potarazu | AI, war in Iran, and the sovereignty struggle over autonomous technology (February 28, 2026)
The reason this happens lies largely in how Medicare calculates payments to private plans. Medicare Advantage insurers are paid based on the “risk score” of each patient — essentially an estimate of how sick the patient is expected to be. The more diagnoses that are documented, the higher the risk score and the larger the payment from Medicare.
Private insurers have strong financial incentives to document as many diagnoses as possible. As a result, beneficiaries enrolled in Medicare Advantage plans often appear sicker on paper than comparable patients in Traditional Medicare, even when their actual health status is similar.
This practice, known as coding intensity, significantly increases payments to Medicare Advantage plans.
A simple example illustrates how the payment system works in practice. Imagine two 72-year-old patients with the same medical conditions — hypertension and mild diabetes. One is enrolled in Traditional Medicare, where physicians are paid for each visit or service. The other enrolls in a Medicare Advantage plan.
Under Medicare Advantage, insurers are paid a fixed monthly amount based on the patient’s risk score, which is calculated from documented diagnoses. Suppose the base payment for a beneficiary in that region is $10,000 per year. If the patient’s documented conditions produce a risk score of 1.0, the plan receives that full $10,000.
But if the Medicare Advantage plan conducts additional chart reviews, in-home health assessments, or data analysis and identifies more diagnostic codes — for example adding conditions such as chronic kidney disease, neuropathy, or vascular disease — the patient’s risk score might increase to 1.2. The payment then rises proportionally to $12,000 per year, even if the patient’s actual health status and medical treatment have not changed.
Multiply that difference across millions of beneficiaries and the impact becomes enormous. Small increases in risk scores — often only a few percentage points — can translate into tens of billions of dollars in additional Medicare spending each year.
Over time, these coding differences add up. Research suggests that risk scores for Medicare Advantage enrollees are often 6 to 16 percent higher than comparable patients in Traditional Medicare.
Another factor contributing to higher payments is favorable selection. Healthier seniors are often more likely to enroll in Medicare Advantage plans, while those with more complex medical needs sometimes transition back to Traditional Medicare. This dynamic can make Medicare Advantage populations appear less expensive than they actually are, further distorting payment levels.
Taken together, these factors have produced a system in which Medicare Advantage costs significantly more than the traditional program it was intended to replace.
These higher payments have a direct and underappreciated consequence: they raise premiums for all Medicare beneficiaries.
Because Medicare Part B premiums are set nationally and designed to cover roughly one-quarter of program spending, higher payments to Medicare Advantage plans automatically increase premiums for everyone — including seniors who remain in Traditional Medicare.
Recent analysis estimates that Medicare Advantage overpayments increased Part B premiums by about $212 per beneficiary in 2025, totaling $13.4 billion in higher premiums that year alone. Over the past decade, these excess payments have added more than $82 billion to the premiums paid by Medicare beneficiaries.
Most of this burden falls directly on seniors themselves. Nearly 70 percent of beneficiaries have their Part B premiums deducted directly from their Social Security checks, meaning higher premiums translate into lower take-home benefits.
In effect, retirees across the country are quietly paying more each month to finance higher payments to private Medicare Advantage plans.
Importantly, responsibility for this situation does not lie solely with insurers.
Private plans are responding to the incentives embedded in the payment system. When federal policy rewards more aggressive coding or allows payment formulas to diverge significantly from underlying costs, insurers naturally adapt their strategies to maximize reimbursement.
Ultimately, the responsibility lies with policymakers and regulators who design and oversee the program.
The good news is that this problem is solvable. Aligning Medicare Advantage payments more closely with Traditional Medicare would immediately reduce unnecessary spending and directly lower premiums for beneficiaries.
Even modest reforms could produce meaningful savings. If payment levels were gradually brought into parity with Traditional Medicare, seniors could save an estimated $2,600 in premiums over the next decade, while strengthening Medicare’s long-term financial sustainability.
Medicare Advantage now covers more than half of all Medicare beneficiaries, and the program has delivered valuable innovations in care coordination and supplemental benefits. The goal should not be to eliminate the program, but to ensure it operates on a level financial playing field.
If policymakers are serious about protecting both Medicare and the retirement income of American seniors, addressing Medicare Advantage overpayments should be an urgent priority.